In a recent blog post, we offered five key takeaways from the Centers for Medicare & Medicaid Services’ (CMS’s) new 1,300-page proposed 2021 Medicare physician payment rule.
Since the release of that rule a few weeks ago, much of our industry’s attention has been focused on the telehealth policy proposals, and more specifically, on which COVID-19 emergency telehealth policies CMS plans to make permanent after the emergency ends. This attention is well-deserved given the critical role that telehealth has played during the pandemic and the key role that CMS’s emergency policies played in enabling the rapid transition to telehealth services earlier this year.
But beyond telehealth, CMS’s new regulation also includes very important Evaluation and Management (E/M) office visit coding, documentation, and payment system reforms that have been several years (if not decades) in the making.
In the 2020 Physician Fee Schedule final rule that was released last November, CMS finalized an overhaul of the five-level documentation, coding, and payment system for Medicare E/M outpatient office visits. To provide the industry time to prepare for such a significant transition, the overhaul was scheduled for 2021, rather than 2020.
Over the past several months, industry stakeholders have speculated as to whether CMS would delay this transition due to the pandemic. In this rule, CMS reconfirmed that the transition will indeed take place next year: “[a}s finalized in the CY 2020 PFS final rule, in 2021 we will be largely aligning our E/M visit coding and documentation policies with changes laid out by the CPT Editorial Panel for office/outpatient E/M visits, beginning January 1, 2021.”
Key elements of this overhaul include:
- Reducing the number of levels to four for new patients by deleting the level 1 visit code 99201
- Retaining five levels of coding for established patients
- Eliminating history and physical exam as requirements for code selection
- Allowing clinicians to choose a visit level based on either medical decision making (MDM) or time*
- Revising time and MDM guidelines for all codes
- Creating a new add-on code for the work associated with visits that are part of ongoing primary or specialty care (GPC1X)
- Creating a new prolonged services code for each additional 15 minutes spent on a patient visit beyond the time required for a level 5 visit (99XXX)
- Adopting new relative value units (RVUs) for each code to amend the payment amount for each code
*For those physicians who want to use time to select a code level for a service, CMS will allow them to do so whether or not counseling and/or coordination of care dominates the service. And for coding purposes, time for these services is not simply the time spent with the patient in the exam room: it is “the total time on the date of the encounter”, including both face-to-face and non-face-to-face time.
As determined by the American Medical Association’s CPT Editorial Panel, time counts would include the following activities when performed by a physician or other qualified billing practitioner on the date of the encounter:
- Preparing to see a patient (e.g., review of tests)
- Obtaining and/or reviewing separately obtained history
- Performing a medically appropriate examination and/or evaluation
- Counseling and educating the patient/family/caregiver
- Ordering medications, tests, or procedures
- Referring and communicating with other health care professionals (if not separately reported)
- Documenting clinical information in an EHR
- Interpreting results (if not separately reported) and communicating results to the patient/family/caregiver
- Care coordination (if not separately reported)
For physician groups, these reforms could be a real gamechanger impacting practice workflows, documentation procedures, clinical staffing models, and reimbursement. Depending on a physician’s specialty and the mix of services they provide, the reimbursement changes could be significant.
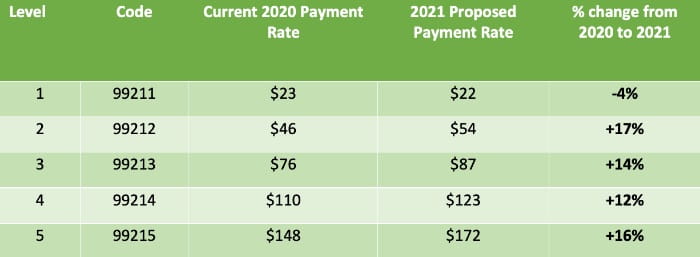
For established patient visits, here are the proposed payment rates for 2021 for each level of E/M visit:
As a result of these changes, medical specialties that primarily provide E/M office visits are likely to see an increase in Medicare reimbursement. CMS projects a 13% increase for family practice and a 14% increase for oncology.
However, because overall Physician Fee Schedule spending must meet certain budget neutrality rules established by Congress, these increases in E/M payment rates triggered a nearly 11% cut to the overall Medicare 2021 conversion factor. For specialties that do not primarily provide E/M visits, this is likely to result in a substantial decline in Medicare reimbursement. CMS projects a 7% cut for general surgery and a 11% cut for radiology next year.
In response, certain medical societies and physician trade associations are pushing back hard against these proposed cuts and are asking CMS and Congress to make for further changes. Following the close of its customary public comment period in early October, CMS is scheduled to issue its final 2021 Physician Fee Schedule rule in late November. With the January 1, 2021 implementation date following shortly thereafter, physician groups should start preparing for these changes as soon as possible. A good place to start would be with the AMA CPT Editorial Board’s official guidance document, which can be found here.